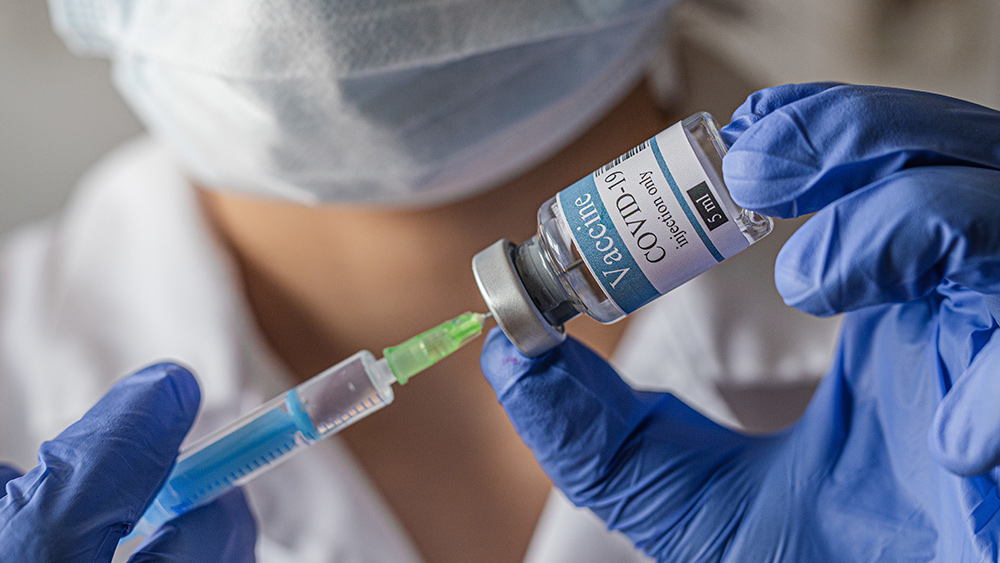
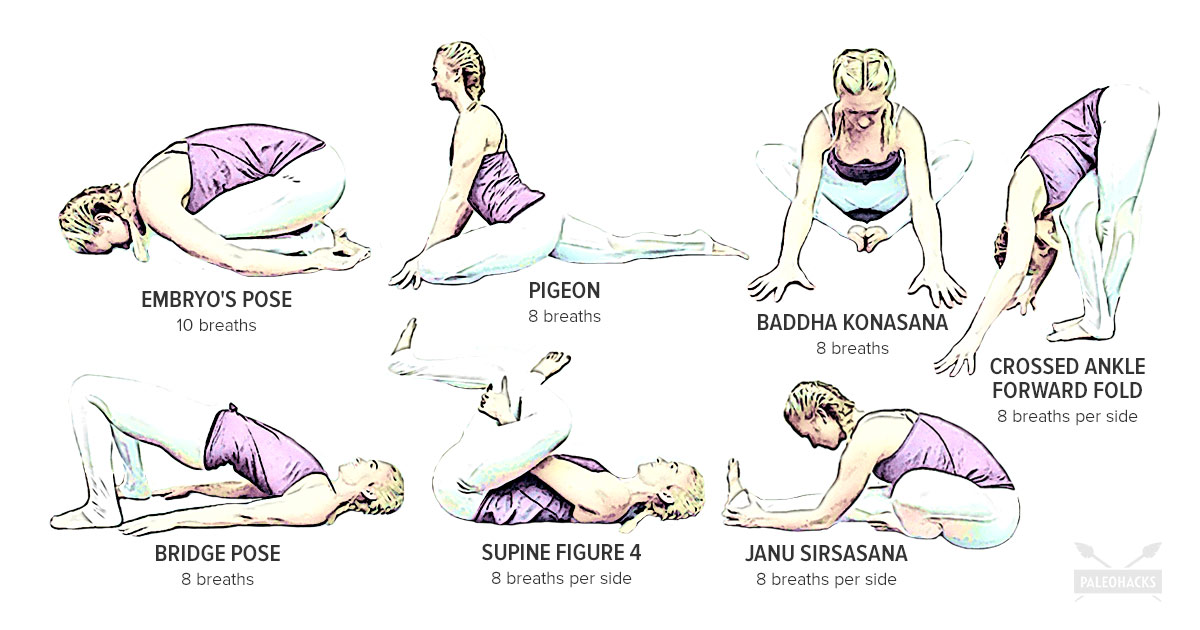
"They are a super picky eater. They won’t eat vegetables."
These are some of the most common words I hear from the parents of my autistic patients.
Dietary aversions and preferences
Of course, we all know that eating our veggies is healthy, but for a child on the spectrum what the bacteria would do with that fiber can have a massive impact on how their immune system and brain work. There can be a few reasons they might dislike these types of foods. They may have too many bacteria in the small intestine due to poor bowel motility and they could cause pain and bloating.
There could also be the possibility that a child on the spectrum could have their parietal lobes affected. This could lead to an aversion to the texture as well as the taste. Since there is typically altered sensory perception with a child on the spectrum this can include the lips and tongue, which have a lot of real estate on the homunculus, or the taste themselves.
Also, the concept of exorphins is where certain foods can activate opioid receptor sites, literally making a child addicted to the very foods that has the potential to be the most problematic. When a parent asks me what foods their child should avoid, I typically ask them what foods they seem addicted to and we have some of the answers.
https://www.ncbi.nlm.nih.gov/pubmed/27065833
Immune system, Autism, and microbiome
Although the research is still being done, it is becoming more apparent that either the child themselves or the mother suffers from a pattern of immune activation that can lead to disrupted gut barrier, which can contribute to an alteration in not only bacteria, but as well as how the immune system in the brain responds to immune insults and the proper development of the nervous system.
Since bacteria are responsible for metabolization of foods, extracting nutrients, building neurotransmitters, and modulating immune function, this can lead to an inflammatory cascade and cycle. The diet can become narrower, bring further nutrient depletion, cause more of a microbial imbalance, all of which cause more of a pro-inflammatory environment.
Although most people with chronic disease have some form of inflammatory response, researchers have eluded that when a subset of immune cells called TH17 are brought into the mix either in a pregnant woman or an autistic child themselves, now we can see this can drive the inflammatory response so imbalanced that a neurodevelopmental disease is more likely to develop.
https://www.ncbi.nlm.nih.gov/pubmed/30251184
https://www.ncbi.nlm.nih.gov/pubmed/30523646
Bacteria, fiber, and immune modulation
When bacteria eat fiber, they make different compounds called short-chain fatty acids (SCFA) that can totally affect how the central nervous system works by activating several parts of the enteric nervous system. Some of the fancy words are ‘G-protein coupled receptors’ and ‘histone deacetylases’… with the latter being a way that gene expression is modulated with the catch-phrase ‘epigenetics’ and now the brain’s function can start to change. There is even data demonstrating that this can lead to an increase in oral tolerance, so the immune system won’t target foods as ‘bad guy.’
The concept of oral tolerance is where the immune system is told to ignore foods that are being consumed so they don’t contribute to an inflammatory response. This can be a large catch-22 in the sense that the less diverse a child’s diet, typically the lower their oral tolerance of foods, so unfortunately, the immune system and microbiome get painted into a corner that can be difficult to get out of.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4855267/
https://www.ncbi.nlm.nih.gov/pubmed/27332875
In particular, one SCFA called butyrate seems to take the gluten-free cake. Not only is butyrate a primary energy source for cells in the large intestine to ‘fix the gut’, but it also has a great impact on the immune system healing the gut lining. It also helps fight the bad bacteria that can be driving the immune issues in the first place. Butyrate helps turn off pro-inflammatory signals as well as turn on anti-inflammatory signals and bring balance back to the immune system by helping with something called T-regulatory cells which can really help with doing exactly what they sound like they do, regulate the immune response.
This is especially important given that the brain and GI tract are in constant communication, not only via the vagal nerve, but the sympathetic nerve fibers send signals directly to the brain. Given that the microbiome and inflammatory cytokines are an important part of this relay system, their involvement with something like Autism shouldn’t be ignored.
For those of us that have been doing this enough, it is blatantly apparent that there is immune system involvement, with some articles showing upwards of 70% of children on the spectrum have an autoimmune disease process going on in their brain. Hence, to help modulate the altered immune response, the bacterial by-products of fermenting fibers can go a long way in helping bring balance to the immune response, gut lining, and nervous system.
https://www.ncbi.nlm.nih.gov/pubmed/26868600
https://www.cell.com/cell-host-microbe/fulltext/S1931-3128(15)00169-9
https://www.ncbi.nlm.nih.gov/pubmed/28636959
https://www.ncbi.nlm.nih.gov/pubmed/15546805
https://www.ncbi.nlm.nih.gov/pubmed/7682457
https://www.ncbi.nlm.nih.gov/pubmed/25981892/
https://www.ncbi.nlm.nih.gov/pubmed/30523646
Although only one piece of the puzzle, giving the gut and immune cells of a child with ASD what they need can really help. But on the back end, a large goal is to have these kids lose their taste aversion and start eating veggies and other healthier foods. To accomplish this, we have to address the root causes of their food aversions. This means addressing proper magnesium levels of the brain and rebalancing gut microbiota.
https://www.ncbi.nlm.nih.gov/pubmed/23474371
Once we see how all the pieces are connecting, we can paint the clearest picture possible. Since each child is unique, each picture is unique as well. The good news is, once a path to healing is identified in a child, the effect can snowball in the sense that the fewer food aversions a child has, the better the gut and immune system work, so the better the brain works, so the more foods they will eat, and the cycle continues

 www.naturalnews.com
www.naturalnews.com